http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3165955/
The endocannabinoid system is implicated in a variety of physiological and pathological conditions (inflammation, immunomodulation, analgesia, cancer and others). The main active ingredient of cannabis, Δ9-tetrahydrocannabinol (Δ9-THC), produces its effects through activation of CB1 and CB2 receptors. CB1 receptors are expressed at high levels in the central nervous system (CNS), whereas CB2 receptors are concentrated predominantly, although not exclusively, in cells of the immune system. Endocannabinoids are endogenous lipid-signalling molecules that are generated in the cell membrane from phospholipid precursors. The two best characterized endocannabinoids identified to date are anandamide (AEA) and 2-arachidonoylglycerol (2-AG). Here we review the relationship between the endocannabinoid system and anti-tumour actions (inhibition of cell proliferation and migration, induction of apoptosis, reduction of tumour growth) of the cannabinoids in different types of cancer. This review will focus on examining how activation of the endocannabinoid system impacts breast, prostate and bone cancers in both in vitro and in vivo systems. The therapeutic potential of cannabinoids for cancer, as identified in clinical trials, is also discussed. Identification of safe and effective treatments to manage and improve cancer therapy is critical to improve quality of life and reduce unnecessary suffering in cancer patients. In this regard, cannabis-like compounds offer therapeutic potential for the treatment of breast, prostate and bone cancer in patients. Further basic research on anti-cancer properties of cannabinoids as well as clinical trials of cannabinoid therapeutic efficacy in breast, prostate and bone cancer is therefore warranted.
LINKED ARTICLES
This article is part of a themed issue on Cannabinoids in Biology and Medicine. To view the other articles in this issue visithttp://dx.doi.org/10.1111/bph.2011.163.issue-7
Introduction
Cancer resulted in approximately 7.6 million deaths worldwide in 2008 (Ferlay et al., 2010). An estimated 12.7 million new cancer cases were diagnosed in 2008 alone (Ferlay et al., 2010). Worldwide, an estimated 1.38 million women and 914 000 men were diagnosed with breast and prostate cancer, respectively, in 2008 (Ferlay et al., 2010). If this trend continues, cancer will overtake heart disease and become the predominant cause of death (Heron et al., 2009). Effective treatment and management of cancer is critical for cancer patients but the development of safe and effective treatments that improve cancer therapy remains an unmet need. Cannabinoids and modulators of the endocannabinoid system have recently been shown to produce anti-tumour actions (reduction of inflammation, cell proliferation and cell survival properties) in different models of cancer. The present review focuses on breast, prostate and bone cancer in which links to the endocannabinoid system have been studied. More work is necessary to determine whether pharmacotherapies targeting the endocannabinoid system improve the treatment of cancer in patients.
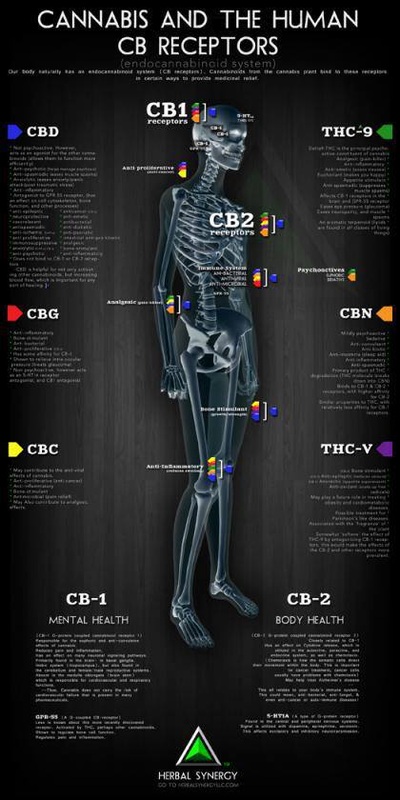
Cannabinoids are implicated in a variety of physiological and pathological conditions including inflammation, immunomodulation, analgesia, cancer and others (for reviews Pacher et al., 2006; Di Marzo, 2008). The main active ingredient of cannabis, Δ9-tetrahydrocannabinol (Δ9-THC), produces its effects through activation of G-protein-coupled CB1 (Matsuda et al., 1990; Ledent et al., 1999; Zimmer et al., 1999) and CB2 (Munro et al., 1993; Buckley et al., 2000) receptors. Endocannabinoids are endogenous lipid-signalling molecules that are generated in the cell membrane from phospholipid precursors. They bind and activate one or more cannabinoid receptor subtypes, thus producing cannabimimetic properties (for reviews Piomelli, 2005; Di Marzo, 2006). The two best studied endocannabinoids isolated to date are anandamide (AEA) and 2-arachidonoylglycerol (2-AG). Anandamide is hydrolysed by the enzyme fatty-acid amide hydrolase (FAAH) whereas 2-AG is degraded predominantly, although not exclusively, by monoacylglycerol lipase (MGL) (for reviews Pacher et al., 2006; Jhaveri et al., 2007; Guindon and Hohmann, 2009; Wang and Ueda, 2009). Thus, enzymes catalysing endocannabinoid hydrolysis represent potential new targets for cancer pharmacotherapies. In this review, drug and molecular target nomenclature conforming to British Journal of Pharmacology Guide to Receptors and Channels (Alexander et al., 2009) has been employed. Here, we will refer to effects of cannabinoids blocked by CB1 antagonists (SR141716A, AM251) as being CB1-mediated and effects blocked by CB2 antagonists (SR144528, AM630) as CB2-mediated.
Cancer is marked by uncontrolled cell division and cell death emerging from cumulative damage of important regulatory genes. Multiple genes likely need to be damaged in order for a cancer to grow and develop the ability to spread (i.e. metastasize). Cancers may be hereditary and/or caused by external (tobacco, chemicals, radiation, infectious organisms and others) and/or internal (inherited mutations, hormones, mutations from metabolism and others) factors. This review will focus on uncovering connections between the endocannabinoid system and breast, prostate and bone cancers with an emphasis on understanding how these connections could be exploited for their therapeutic anti-cancer potential.
Animal models of cancer have been developed to experimentally assess pathophysiological mechanisms implicated in the analogous clinical syndrome. These models provide insight into pathophysiological processes of the disease state and elucidate mechanisms of action that may be targeted by drug discovery efforts aimed at identifying novel therapeutics. These models thus permit preclinical evaluation and validation of therapeutic efficacy of new pharmacotherapies.
Anti-proliferative properties of cannabis compounds were first identified 35 years ago. Here, it was first shown that administration of Δ9-THC inhibits lung adenocarcinoma cell growth in vivo (i.e. after oral administration in mice) and in vitro (Munson et al., 1975; Carchman et al., 1976). It took more that two decades before the potential anti-tumour properties associated with a cannabinoid were investigated further. In the past 14 years, an emerging body of research, primarily employing in vitro models of different cancers, has helped elucidate the mechanisms through which cannabinoids and the endocannabinoid tumour system influences cancer cell proliferation, migration and apoptosis (i.e. programmed cell death).
The mechanisms through which cannabinoids/cannabinoids receptors impact proliferation, migration and apoptosis of cancer cells are quite complex and our understanding of these processes remain incomplete. Moreover, these mechanisms differ in different types of cancer, and both pro- and anti-apoptotic effects of cannabinoids have been reported. A schematic representation of the major signalling pathways that are implicated in the activation of different cannabinoid receptor subtypes through their agonists and their involvement in these processes is summarized in Figure 1. (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3165955/figure/fig01/)
Several mechanisms are likely to underline the pro-apoptotic effects of cannabinoids and explain their anti-cancer effects. Cannabinoids induce de novo synthesis of ceramides, a family of lipid molecules composed of sphingosine and a fatty acid, found in the cell membrane. Synthesis of ceramide occurs via activation of the enzyme ceramide synthase and leads to downstream activation of an extracellular regulated kinase (ERK) signalling cascade. This process results in cell cycle arrest and apoptosis. Activation of either CB1 or CB2 receptors triggers the ceramide-ERK signalling pathway to promote apoptosis (Kogan, 2005; Sarfaraz et al., 2006, 2008) (Figure 1). The increase in ceramide can also activate the p38 mitogen-activated protein kinase (p38MAPK) pathway which can lead to apoptosis through multiple mechanisms (i.e. through activation of cysteine proteases (i.e. caspases) or through cytochrome C release from mitochondria). The sustained activation of ERK also promotes the induction of cyclin kinase inhibitor (p27/KIP1) which modulates regulatory molecules of the cell cycle (cyclins, cdks) resulting in cell cycle arrest and apoptosis (Kogan, 2005; Sarfaraz et al., 2006, 2008) (Figure 1). Cell cycle arrest involves the up-regulation of the p53 protein which will differentially alter levels of pro- and anti-apoptotic proteins (i.e. increase the levels of the pro-apoptotic protein Bax and lower the levels of the anti-apoptotic protein Bcl2, respectively, thereby shifting the ratio towards Bax) which ultimately leads to activation of caspases that play an essential role in triggering apoptosis (Sarfaraz et al., 2006). Activation of either CB1 or CB2 receptors also inhibits adenylyl cyclase (AC) activity and lowers both cyclic adenosine monophosphate (cAMP) levels and protein kinase A (PKA) activity, thereby causing down-regulation of gene transcription, leading to apoptosis (Guzmán, 2003; Kogan, 2005; Bifulco et al., 2008; Sarfaraz et al., 2008). Activation of transient receptor potential cation channel V1 (TRPV1) receptors also leads to increases in intracellular levels of both hydrogen peroxide (H2O2) and/or calcium or the release of cytochrome C from mitochondria, causing apoptosis through both distinct and overlapping mechanisms (Figure 1) (Maccarrone et al., 2000).
Cannabinoid receptor 1 ligands have pro-apoptotic properties, in part, through inhibition of the Ras protein (p21ras) which is involved in inducing DNA synthesis (Bifulco et al., 2001). However, CB1 receptor activation can also trigger activation of different tumour cascades that are linked to promotion of cancer cell survival and inhibition of apoptosis. Indeed, CB1 ligands also stimulate the PI3K/PKB tumour pathway, an essential tumour pathway implicated in cell survival. Activation of PI3K/PKB downstream of CB1 activation may promote apoptosis either directly or through inhibition of p27/KIP1 (Gómez del Pulgar et al., 2000; Sarfaraz et al., 2008). Thus, both pro- and anti-apoptotic effects of cannabinoids have been reported, raising the possibility that a dysregulation of the endocannabinoid system may also contribute to cancer/tumour development. However, activation of ERK downstream of cannabinoid receptor activation also promotes anti-cancer effects through inhibition of cancer cell migration (Blazquez et al., 2003; Kogan, 2005). More work is necessary to determine the balance between these various mechanisms, and how they modulate cancer in vivo.
Phytocannabinoids may also interfere with the ability of lysophosphatidylinositol (LPI), a putative endogenous ligand for G-protein-coupled receptor 55 (GPR55), to promote cancer cell proliferation through activation of the putative novel cannabinoid receptor subtype (Figure 1). Pretreatment of breast and prostate cancer cells with cannabidiol, a major component of marijuana, or with SR141716A (a CB1 antagonist that also possesses agonist/antagonist properties at GPR55), blocks the ability of LPI to induce cell proliferation through GPR55, thereby producing anti-cancer effects (Piñeiro et al., 2011). Activation of GPR55 by LPI promotes cancer cell proliferation following activation of distinct intracellular tumour cascades [i.e. ERK, AKT and calcium mobilization (Piñeiro et al., 2011)]; these anti-proliferative effects were also blocked using siRNA for GPR55.
Cannabinoids in clinical cancer studies:
Cannabinoids have been evaluated in cancer patients for their anti-emetic, anti-nociceptive and orexigenic properties. Numerous studies have been published documenting the anti-emetic properties of cannabis-like compounds (Davis, 2008; Navari, 2009; Parker et al., 2011 for reviews). Fewer clinical trials have evaluated pain relief following cannabinoid administration in cancer patients. Indeed, the role of cannabinoids in relieving pain associated with cancer has been evaluated in only five clinical studies. Four of these studies were performed more than 32 years ago (Noyes et al., 1975a,b; Jochimsen et al., 1978; Staquet et al., 1978; Johnson et al., 2010). In the initial study, oral THC, at doses of 15 and 20 mg, produced analgesic effects in patients experiencing cancer pain (Noyes et al., 1975a). The same study showed that oral administration of single lower dose of Δ9-THC (10 mg) to patients with cancer pain was well-tolerated and produced a mild analgesic effect, whereas higher doses of Δ9-THC (20 mg) also produced adverse side effects (Noyes et al., 1975b). Another study, using a nitrogen analogue of Δ9-THC, showed that pain relief was superior to placebo in patients with cancer (Staquet et al., 1978). Another group, also using a nitrogen analogue of Δ9-THC, showed that the cannabinoid (2 or 4 mg) was not effective as an analgesic, compared with placebo and even appeared to augment pain perception in patients with chronic pain due to malignancies (Jochimsen et al., 1978). A more recent study demonstrated that the administration of Sativex (Δ9-THC: CBD in a 1:1 ratio) reduced pain scores when compared with placebo, whereas effects of Δ9-THC administration alone on pain did not reach significance (Johnson et al., 2010).
The present studies suggest that additional clinical trials evaluating the therapeutic efficacy of cannabinoids in cancer pain are warranted, particularly in light of other aspects of cannabinoid receptor pharmacology that hold considerable therapeutic potential (i.e. anti-emetic and anti-tumour properties).
Conclusion and limitations:
The available literature suggests that the endocannabinoid system may be targeted to suppress the evolution and progression of breast, prostate and bone cancer as well as the accompanying pain syndromes. Although this review focuses on these three types of cancer, activation of the endocannabinoid signalling system produces anti-cancer effects in other types of cancer including skin, brain (gliomas) and lung (Velasco et al., 2007; Bíróet al., 2009; Pacher and Mechoulam, 2011 for reviews). Interestingly, cannabis trials in population-based studies failed to show any evidence for increased risk of respiratory symptoms/chronic obstructive pulmonary disease (Tan et al., 2009; Hancox et al., 2010) or lung cancer (Tashkin, 2005) associated with smoking cannabis. Moreover, synthetic cannabinoids and the endocannabinoid system play a role in inhibiting cancer cell proliferation and angiogenesis, reducing tumour growth and metastases and inducing apoptosis in all three types of cancers reviewed here. These observations raise the possibility that a dysregulation of the endocannabinoid system may promote cancer, by fostering physiological conditions that allow cancer cells to proliferate, migrate and grow. These observations also raise the exciting possibility that enhancing cannabinoid tone through cannabinoid-based pharmacotherapies may attenuate these harmful processes to produce anti-cancer effects in humans. However, the basic research findings are far from being completely understood and further research is warranted to better understand the complexity of dynamic changes in the endocannabinoid system in cancer. One of the reasons for this complexity is likely attributable to the highly interactive nature of lipid signalling pathways which recruit different signalling pathways and mechanisms of action. Indeed, endocannabinoids are known to interact with the cyclooxgenase enzyme, inhibit the transcription of genes implicated in metastasis processes, induce cell cycle arrest, activate the formation of reactive oxygen species and ensure the integrity of raft/caveolae needed for anti-proliferative properties. However, other mechanisms are also likely to be involved and interact with the endocannabinoid system in ways that are yet to be discovered.
Many in vitro and in vivo studies have shown that cannabinoids are efficacious in reducing cancer progression (i.e. inhibition of tumour growth and metastases as well as induction of apoptosis and other anti-cancer properties) in breast, prostate and bone cancer. However, further research is needed because the complexity of the effects of cannabinoids and their interaction with other mechanisms and signalling pathways remain to be elucidated. The need for further study is particularly crucial in the case of prostate cancer; only one study, performed in mice, has evaluated in vivo effects of a cannabinoid (JWH-015) on tumour growth. The paucity of in vivo preclinical and clinical data is striking given the large number of compounds that have been tested in vitro in different types of prostate cancer cell lines.
Despite the need for further in vitro and in vivo studies, the literature is nearly unanimous in suggesting that cannabinoids and endocannabinoids reduce the progression of cancer in both in vivo preclinical and in vitro model systems. The need for additional clinical trials of cannabinoid therapeutic efficacy in cancer appears beyond doubt; only few studies have evaluated the effects of cannabinoid in alleviating cancer pain, in contrast to the extensive literature supporting efficacy of cannabinoids as anti-emetics. Furthermore, future research needs to explore the therapeutic potential of multimodal analgesic strategies that combine cannabinoids with other commonly used medications (opioids) or employ multiple phytocannabinoids in combination. The use of different pharmacotherapies in combination may increase the likelihood of synergistic interactions between compounds with multiple distinct mechanisms of action; such combinations may produce a more beneficial therapeutic ratio in cancer patients compared with conventional analgesics, resulting in improved pain relief and anti-cancer effects with fewer adverse side effects. Moreover, because cannabinoids attenuate neuropathy produced by cancer chemotherapy through CB1 and CB2-dependent mechanisms (Rahn and Hohmann, 2009 for review), the possibility remains that cannabinoids in combination with chemotherapy may enhance both anti-tumour actions of chemotherapy and attenuate unwanted iatrogenic side effects (e.g. emesis, neuropathy). Further basic research on cannabinoid anti-cancer properties as well as clinical trials evaluating cannabinoid efficacy in cancer are required before cannabinoid use can be established and accepted as effective adjuncts to cancer therapy...






















































































































 RSS Feed
RSS Feed
